Impact of Medical Technology on Healthcare in Times of Pandemic and Beyond
Digital transformation in healthcare has never been so urgent before. Pandemic has revealed the weaknesses and unpreparedness of the healthcare systems in many countries across the world. Even the states with well-funded and strong healthcare sector were shocked by the unprecedented influx of patients and reported a wide range of pandemic-related issues, such as the shortage of PPE, equipment and medical staff, overwhelming paperwork and poorly developed processes.
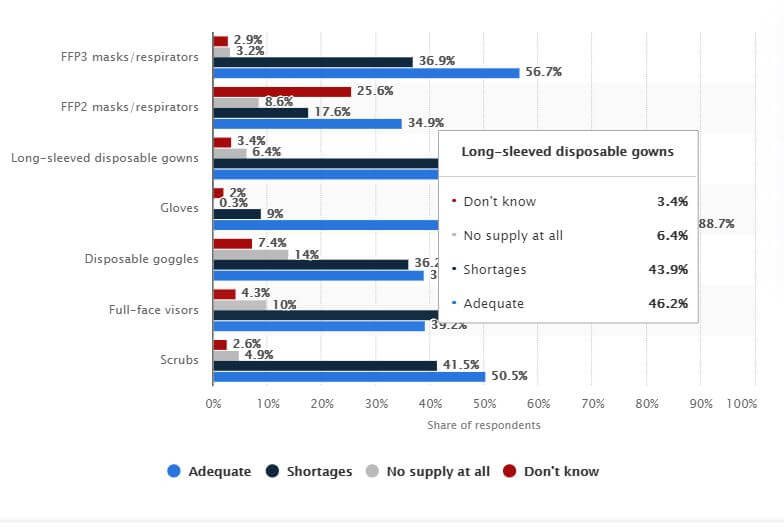
Not surprisingly, digital technologies often successfully address these and other problems in healthcare. After all, it’s digital technology that helps keep our society running in the times of widespread work from home, social distancing and lockdown. Digital technology in medicine, in turn, plays even a more important role for it helps save lives and provide adequate health and social care to millions of people in need.
In this article, we will dwell on the plenty of opportunities of digital transformation in healthcare in times of crisis and beyond.
If you are a healthcare professional, a decision-maker and an innovator in this sector, this article will provide you with several ideas on how to leverage digital technology for the benefits of customers, patients, doctors and staff and the whole industry. If by the end of reading this article you still have some questions unanswered, simply contact our team. We have been building custom medical software for years, worked with different hospitals, pharmaceutical companies, foundations and health tech startups and will be happy to help you.
How can we help?
In the middle of April, UN Department of Economic and Social Affairs issued the new policy brief where the organization emphasized the importance of digital technology in addressing the issues and embracing reality during the pandemic.
“The crisis has demonstrated that it is impossible for societies to ignore technological advancements as they are continuing to change business models and people’s everyday lives. Governments should embrace these policy- and technological developments and harvest the digital opportunities that can support the long-term sustainable development of their countries.” (un.org)
From the very beginning of mass quarantine, the benefits of integrating digital technology into people’s everyday lives became clear. Thanks to digital technology we could work from home, socialize, get the necessary information, exercise and maintain a healthy lifestyle, shop and even get basic medical and mental care.
However, the role of information technology in medicine and healthcare, in general, became particularly critical.
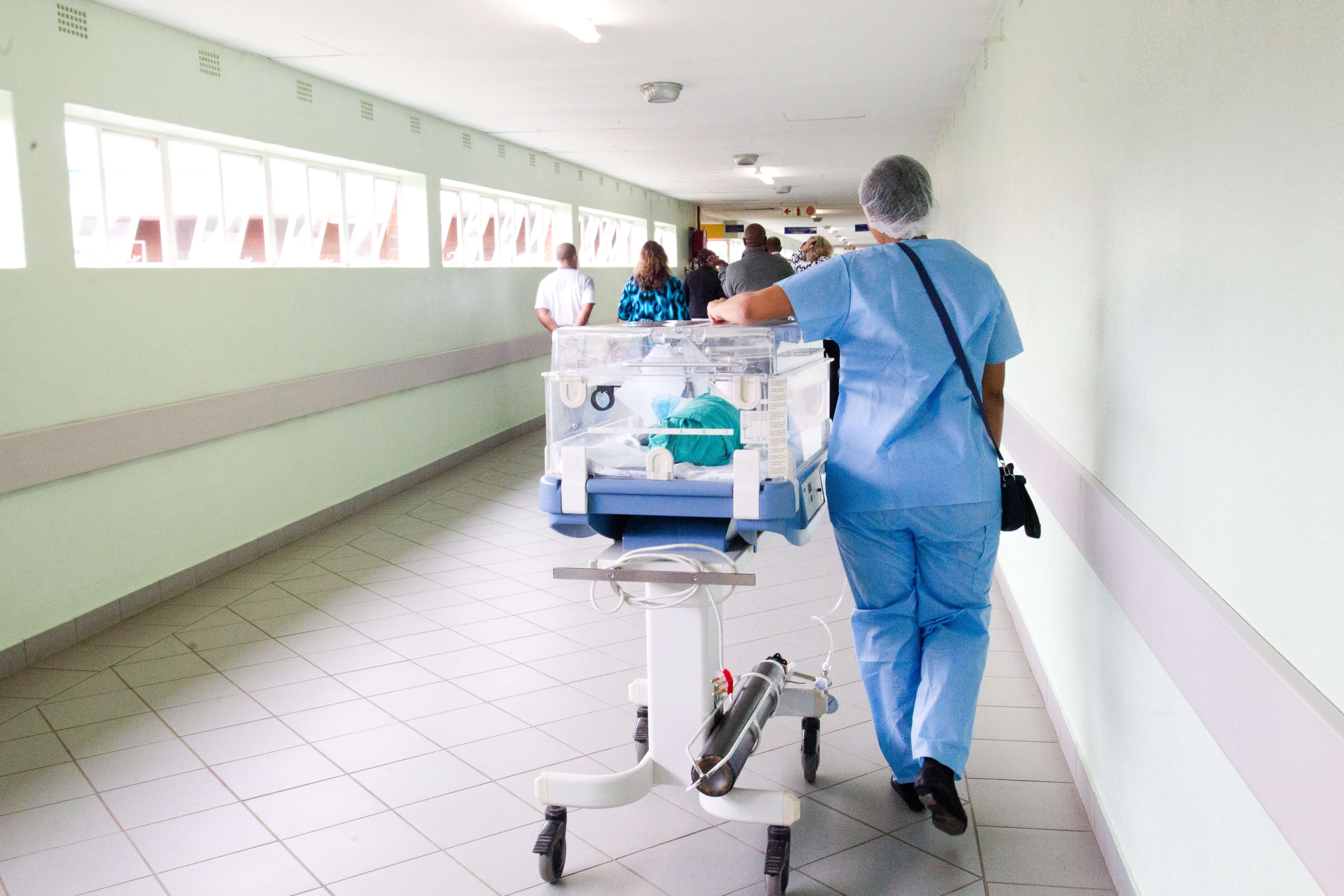
First of all, existing and ubiquitous digital systems in healthcare such as patient tracking devices, RFID and Internet of Things systems for healthcare asset tracking, mobile apps for doctors and patients, EHR and e-prescriptions, telemedicine solutions, etc. could be and are used as the primary tools to address the many risks and issues associated with the crisis in healthcare. Here are just some of the problems these technologies help solve:
Common risks and issues of healthcare systems working under pressure
- Shortages caused by an insufficient supply of PPE, medication, equipment.
- Hectic patient admission/discharge processes caused by the unpredictable patient influx.
- Disrupted medical supply chain at national and global levels.
- Insufficient human resources caused both by huge influx of patients and high rate of infection among healthcare staff.
- Uncontrolled infection spreading.
- Delayed treatment for non-urgent patients.
- Neglected patients with chronic diseases.
- Higher risks of mistakes, undeserving in terms of crisis.
- High pressure on the mental and physical health of medical staff.
Secondly, businesses, governments and world organizations use novel digital solutions to identify problems in healthcare that technology can solve.
Corporations such as Apple and Google and several countries including Norway, Australia, China, Singapore either work on or have already launched different COVID-19 contact tracking apps to keep the spread of the pandemic under control. Governments and agencies allocate serious budgets to speed up innovation in healthcare and help medical facilities and healthcare professionals successfully get over the pandemic crisis. eHealth startups receive massive support and investment. Not to mention all the attention top biotech companies on the vaccine development landscape are getting these days.
The growing interest to digital transformation in healthcare in the context of pandemic and beyond prove the focus on technology in this industry will likely increase in the future. It’s still too early to say how much healthcare product development and digital transformation in this sector will contribute to mitigating this pandemic crisis. However, we can already talk about the positive role of technology in improving healthcare outcomes in the frontline today.

It’s hard to underestimate the importance of technology in healthcare. From EHR and virtual consultations to hospital asset tracking systems, digital tools help make healthcare processes smarter, safer and more efficient.
Implement infection control
Tracking technology such as RFID, RTLS as well as more complex networks of connected devices and spaces help monitor and control people flow (patients, doctors, nurses, other staff), locate medical tools and equipment, track sterilization processes. These technologies are indispensable in identifying infected spots and mitigating infection spread.
Increase efficiency

There’s a whole range of time-proven and widely adopted digital systems for doctors, patients, hospitals in general that help deliver better, safer and more timely healthcare services. Among them are electronic health records, hospital management systems, medical inventory software and e-prescriptions.
These and many other platforms help regulate patient admission and discharge, track treatment effects in real time, improve medication adherence as well as smoothly manage financial, administrative and supply processes behind the scene.
Eliminate human from the process
Commonly used EHR, HMS and e-prescriptions help better organize the very basic processes in health and social care and free staff from time-consuming routine and paperwork. Other emerging technology in healthcare such as wearables, smart hospital equipment, healthcare app for cancer patients, robots and drones completely eliminate human interaction in the cases where it’s possible thus relieving the pressure on the healthcare system and limiting the risks associated with direct contact.
Among good examples are drones delivering medication, self-adjusting vitals tracking hospital beds, autonomous insulin delivery devices, assisting apps for people with mental health issues, etc.
Now let’s dive into a more detailed view of digital transformation in healthcare and see how technology has changed healthcare using real case examples.
Increase patient engagement and medication adherence
Nearly 75% of adults are nonadherent to their medical prescriptions in any way, according to the research conducted by the Polling Company. Mainly, it is caused by various reasons from inability to follow complicated procedures and drug prescriptions to costly treatment and doctor-to-patient communication barriers. The reason for low patient engagement is often lack of easy-to-use tools and channels for patients to connect with doctors and caregivers.
Modern patient engagement and management systems can solve these problems by equipping patients, doctors and healthcare organizations with intuitive cross-channel tools for monitoring, communication and remote consultations.
Optimize patient admission and discharge
Unautomated process of patient rotation, lack of patient tracking systems and inefficient exploitation of ambulance and paramedic resources snowball into delays in hospital discharges and emergency admission slowdown.
Modern tracking and sensor technology in IoT systems should make a game-changing impact on the problem of performance in health and social care. IoT-based patient and facility monitoring and management could become a forward-looking solution for hospitals, ambulance vehicles and care centers.
Globally, 60% of healthcare organizations have already introduced some IoT facilities to their process. Curiously, 42% of industry executives rank monitoring as a primary use of IoT-enabled technology in healthcare. Consider IBM Bluemix-powered solution TMS able to clean the roads for ambulances via smart vehicle tracking and traffic management. Or successfully adopted CSIRO’s Patient Admission and Prediction Tool that analyzes big data to forecast hospital emergency admission with 93% accuracy.
Altogether, the adoption of IoT technology for patient traffic tracking, emergency performance monitoring and smart route management for ambulances should accelerate the admission and discharge processes.
Wearables for people tracking
The wearable market has significantly grown in recent years and became one of the central emerging technologies in healthcare 2020. Today, there is a great variety of wearable devices from affordable connected inhalers to tracking systems for patients used in hospitals.
One of such wearable devices is a medical-grade Biosensor BX100 by Philips that helps remotely track patient vitals including respiratory and heartbeat rate, collect and analyze condition data, detect the risks of deterioration and notify doctors and caregivers in time.
Platforms for patient monitoring

Wearables are not the only important tracking technology that improved healthcare monitoring practices. In fact, in the times of increasing patient flow, large connected systems for patient monitoring in hospitals play even a more important role as they allow significantly unload staff and enable remote continuous monitoring of dozens of ICU patients from one central hub.
One of such unique systems is the product created by the joined efforts of Microsoft and GE Healthcare. Its launch was speeded up on the wave of the pandemic. The system allows managing a 100-bed intensive care network with only several nurses and doctors on-site and significantly reduce the use of PPE.
Artificial intelligence for early diagnosis
AI technologies like computer vision and deep learning are considered some of the most promising technological advancements used in healthcare for early diagnostics. Among recognized applications are automatic skin cancer classification and early pneumonia diagnostics and classification.
Machine learning in preventive medicine
Not only can AI applications in healthcare be used in the diagnostics, but also help identify the problem before it shows. For example, a tech giant Cognizant used machine learning and data analytics to elaborate preventive care practices. Using advanced algorithms, the company was able to identify the early signs of emerging drug addiction among high-risk patients by analyzing their health records, physician’s notes and behavioral patterns.
Mobile apps for doctors and patients
Hardly would we call the benefits of mobile technology in healthcare undiscovered or novel. But new challenges provide new ideas for healthcare mobile apps. Earlier, we have already mentioned the growing interest in contact-tracking apps which could have become popular only in the unique situation of the pandemic. At the same time, many mobile systems for doctor-patient communication and treatment tracking, medication adherence, telemedicine, etc. have been gaining attention and receiving serious support and funding.
Read: Medication calendar app and engagement tool for patients who undergo chemo
Among them is Doximity telemedicine app that helps quickly and safely transfer patient data among healthcare professionals, enable secure patient-doctor communication, manage patient updates, and more.
Digital in-home care
In times of crisis in healthcare, people with chronic conditions and mental health issues become particularly vulnerable. Even if they are not affected by the virus directly, they are most probably underserved and have to miss necessary doctor appointments for safety reasons.
In this case, digital tools for in-home care become important if not the only means of support for such people. Among such tools are Tomorrow Health’s system for in-home care supply, Forward at Home biometric kit for remote care and How Do I? platform that helps people with different conditions including dementia, Alzheimer and learning disabilities maintain a self-sufficient living.

We offer our clients leverage Digiteum tech expertise in the healthcare sector. We’ve delivered a number of digital systems for enterprise-grade pharmaceuticals (Merck, Takeda, Sanofi), hospitals (OLVG), health tech companies (Nextgate, everywhereIM), innovative startups (How Do I?) and foundations (Focus on Lymphoma).
If you are looking for a skilled tech partner who could help you create an actionable plan on how to create SaaS healthcare app or design and deliver a digital system based on your ideas, you are in the right place. Contact our team right away and let’s start working on your project.
Conclusion
We found ourselves in a stressful period full of uncertainty and unpredictability. But pandemic is a rare thing, while a healthcare crisis caused by the leaps in patient influx is seasonal, predictable and, therefore, controllable.
Digital transformation in healthcare is one of the major steps to take in order to keep increasing the pressure under control and help prevent the healthcare crisis entirely.
Interested in implementing new technology in healthcare and looking for an experienced team to work on your ideas? Contact Digiteum.
Contact Digiteum