Key Takeaways from Eyeforpharma Conference
Annual North America’s conference eyeforpharma 2018 was truly one of the most significant events in the industry this year. To my mind, going to Philly and attending this event was more than just a good idea.
This conference allowed me to actively participate and engage in various panels and talks on the pressing problems in the field, meet industry leaders and influencers across different verticals, and most importantly, outline major concepts and issues that today determine the focus and development of pharma and healthcare in general.
Here are my key takeaways from eyeforpharma conference that raise important questions: current state and prospects of patient engagement, the future of pharma strategy and the role of technology and innovation in this course.
- Patient engagement is one of the most focused and widely-discussed topics in pharma today. However, the true nature and understanding of this concept still gets various opinions and remains unclear.
- Patient engagement is a complex concept, therefore, it takes the whole range of efforts that combine management, technology, infrastructure and data solutions to promote patient engagement and create patient-centric care experiences.
- Today, data brings up new opportunities for pharmaceutical practices, healthcare experience and relationship between patients and HCPs. To unlock these opportunities, we need to embrace innovation, introduce relevant digital experiences into our practices and rethink traditional healthcare processes with patient-centric approach in mind.
Now, I would like to explain these points in more details.
Understanding patient engagement
Understanding this concept starts with the very basic definitions, which to my surprise, differ and receive various interpretations. For instance, Evariant sees patient engagement as the bridge between patients and healthcare providers built on trust and deep knowledge of patients as individuals, “their unique habits, wants and needs – both clinical and non-clinical.”
I totally agree. Trust is a must-have throughout healthcare experience. But I don’t think trust is enough to activate patients to engage into their care. Meanwhile, low patient activation is one of the core reasons of poor patient engagement.
Alternative interpretation by Solutionreach extends patient engagement concept to reliable and open communication between healthcare parties. This idea is based on the study that reveals 5 things patients consider the most important for them. They talk about involving patients into their care process, attentive listening to patients, treating a patient as a person and showing respect to both patients and their families. In other words, this understanding of patient engagement focuses on the principles of value-based care where HCPs actually listen to patients, devote their time to address patient’s fears and work on relationships with patients during the lifetime of care experience.
I find this interpretation more complete, as it reflects my idea of patient engagement: trustful reliable relationships between patients and healthcare system, where patients, doctors, hospitals and pharma work as partners to enable successful experience for every party.
At eyeforpharma, this understanding of patient engagement appeared a key interpretation across different panels and discussions. In particular, Ryan Doyle, VP Health Strategy at Idea Couture contrasted Cold and Warm care practices and explained why outcome-focused Cold care doesn’t reflect the needs of today’s patients.
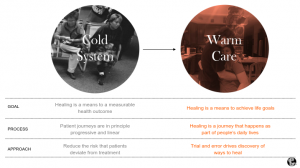
Slide from the presentation at eyeforpharma Philadelphia 2018, Ryan Doyle, Idea Couture.
According to Ryan, patients are still disconnected from their treatment because traditional healthcare experience is impersonal and focuses on clinical outcomes, rather than patients’ life goals. Instead, we need to “reinvision what it means to engage with patients” and introduce healing as the core of every care experience. We need to integrate people into their healing process, make healing a part of people’s lifestyle, listen to patients and create partnerships.
Read: Key takeaways from GBS Forum
Embodying innovation
In order to implement the change proposed by Idea Couture, we need to ignite a new wave of innovation – build infrastructure and introduce a range of solutions and practices for efficient patient engagement.
Another panelist at eyeforpharma, Global Head of Digital Medicines at Sanofi, Bozidar Jovicevic, named some major steps of this transformation and showed the need to build “around-the-pill offering” that could improve healthcare results.
Jovicevic pointed out how important it is to build the infrastructure of tools and services that improve adherence and help patients follow their treatment.
It can be a mobile app like CF Medication that encourages patients to adhere to their medication and allows doctors to follow treatment process remotely, a single chatbot that reminds patients to take their pills or collect feedback on side effects, or even a complex infrastructure with digital solutions able to manage the whole cycle of healthcare experience like the one introduced by Kaiser Permanente.
Sanofi executive also focused on the center of the healthcare system – digitally native patients – and the need to address the needs of progressive, dynamic and tech-savvy customers with relevant digital solutions built with a “design thinking” approach.
Finally, Jovicevic draw attention to communication channels and pointed out the importance of developing effective connections between HCPs and patients.
An illustrative example of such connecting solution is a ChemoDiary app for Merck & Co. This app encourages patients to self-track their reaction to medication and share personalized reports on their conditions with authorized HCPs. As a result, doctors receive relevant, up-to-date information on how patients react to chemo and can remotely follow every step of a complex treatment process.
Unleashing the power of data
At eyeforpharma this year, data became the focus of many panels on care experience and patient engagement. In today’s world, data is already a driving force in many industries. It’s evident, healthcare should not be an exception.
One of the panels was specifically dedicated to the power of data and advanced analytics. Panelists discussed:
- how data-driven solutions can transform customer experience in healthcare,
- what impact data has on different parties of healthcare experience – pharma, doctors, patients and caregivers,
- why pharma should listen to data, act on it and transform data into actionable insights, and
- how patients can expand their participation in care process by sharing data – passive data collected by wearables (i.e. heartbeat rate), personal feedback on medication and treatment and other real world evidence.
The questions raised create actionable milestones on leveraging data in healthcare. However, to my mind, it’s not less important to understand how to implement these promising plans, how to apply practical solutions – digital, infrastructural, operational – able to unleash the power of data in this industry.
In my experience, working with data, especially when it comes to heterogeneous big data, poses a range of issues to solve. In most cases we are dealing with a massive amount of dirty data coming from multiple sources. Parts of this data can be sensitive and requires a certain level of security and high accuracy.
The very same problems relevant to healthcare data were discussed at the panel. For example, real-world evidence, bottomless storage of valuable healthcare information, is usually unstructured and semi-structured data coming from different sources – EHR, personal trackers and health apps, health reports, medical charts and image repositories and even social media. At the same time, 20-year old HIPAA regulations oversecure some of this data, cut access to valuable insights and thus hamper efforts to build data-driven patient experience. And finally, analysis, interpretation and representation of data insights lack established practices and require proper detailing.
Issues associated with heterogeneous data are complex, but not unsolvable. For example, at my company, we have already come across similar problems and managed to deliver working solutions for extracting value from such data.
Working and providing agile delivery services to for Oxford Languages, we had to learn how to collect, sort out, process, analyze, store and represent all types of unstructured and semi-structured lexical data – multilingual dictionary entries, news reports, articles and research papers in massive volumes. Our goals were to develop digital solutions able to efficiently transform multiformat data into clean actionable information at the output with high accuracy, at top speed and as little cost and human effort involved as possible.
As a result, we developed Research Track – web system able to collect field-specific publications, filter this information to provide system users – researchers and scholars – with well-structured compilations on indicated topics.
Another solution, Dictionaries Conversion Framework, allows to transform semi-structured data in different formats – dictionary entries – into well-structured online dictionaries at unprecedented speed with close to 100% accuracy at the output.
And finally, one more data solution, Super Corpus Platform, is able to process a massive volume of raw lexical data – up to 8.6 million documents – in only 24 hours. This system takes one-day worth of news feed in English collected throughout the entire Internet and in 3 hours creates a structured annotated dataset.
All these systems might as well be adjusted to work on health-related data – semi-structured EHR and doctor records, unstructured medical research articles and papers, trial reports, feeds from social media, patient feedbacks in health apps and patient portals, and ever real-time data coming from wellness trackers and other wearables.
In other words, companies that develop a data processing software could help doctors, pharma companies, associations and hospitals retrieve valuable information hidden in health data and start a journey to more a progressive, data-driven healthcare experience.